-
 Leann Macrae-Turuwhenua
★★★★★
2 months ago
Leann Macrae-Turuwhenua
★★★★★
2 months ago
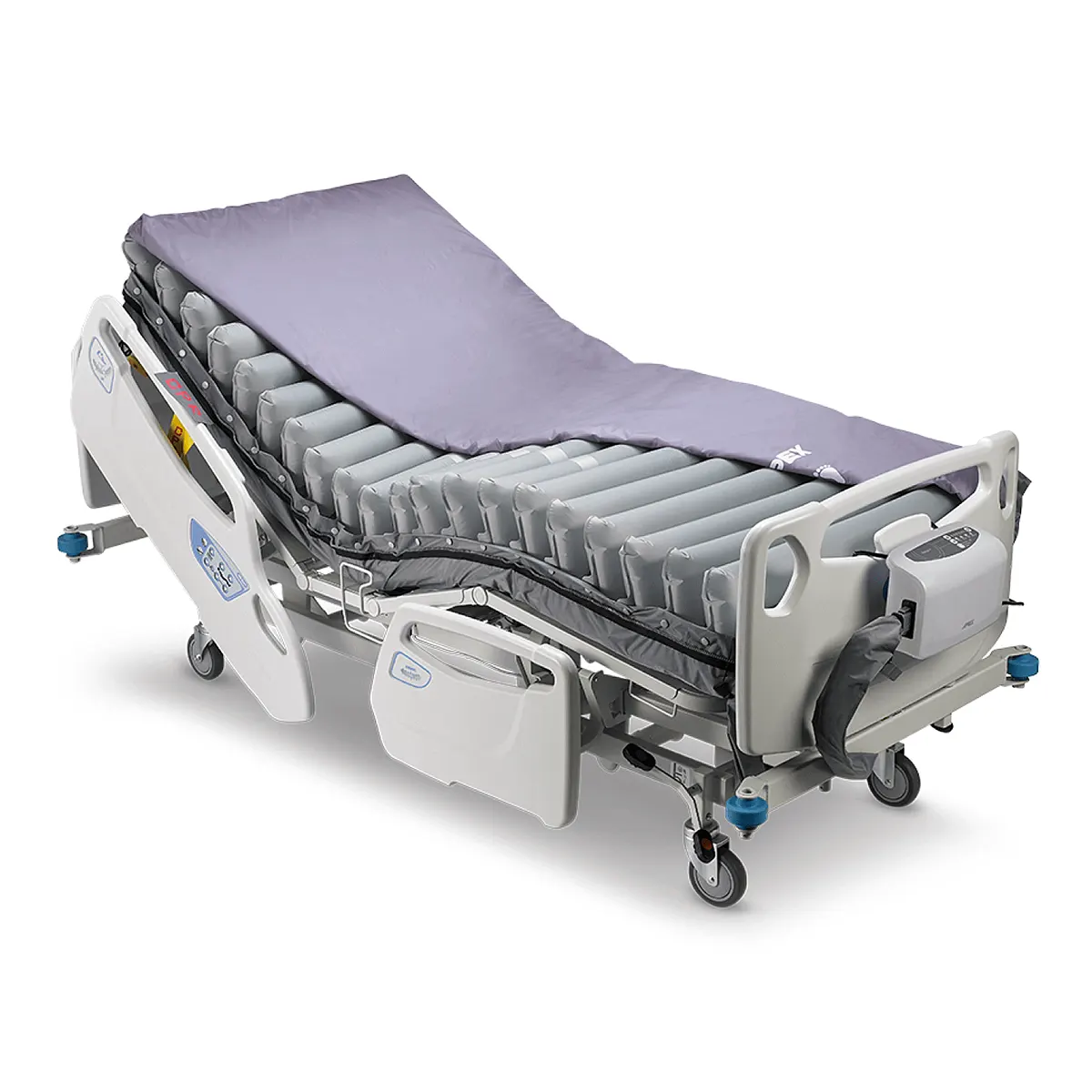
Easy to navigate website. Product delivered within days, which was a great help as was needed. Easy for my husband put together, as he is not the handiest of handymen, that used to be my job. It fits … More well into our small ensuite and can be used by either of us without being inconvenienced. Overall great purchase. No issues. Thanks for following up on this.
-
 Naum Khershberg
★★★★★
a month ago
Naum Khershberg
★★★★★
a month ago
I have purchased the double tubed stethoscope for my son. He is studying nursing @ Federation UniHe really loved the scope and using it every time.Looking professional as well ....I chosen that one because … More one nurse i consulted said that when tube goes to each ear , the quality of sound is better and for the student - it is a great tool.by the way ... also i purchased a case for that thing - great quality ... awesome too.Prices great !!!This product is a bloody bargain .... saved $120 !!!Love you all .... thgank you for the bargain
-
 Mary Reddish
★★★★★
2 weeks ago
Mary Reddish
★★★★★
2 weeks ago
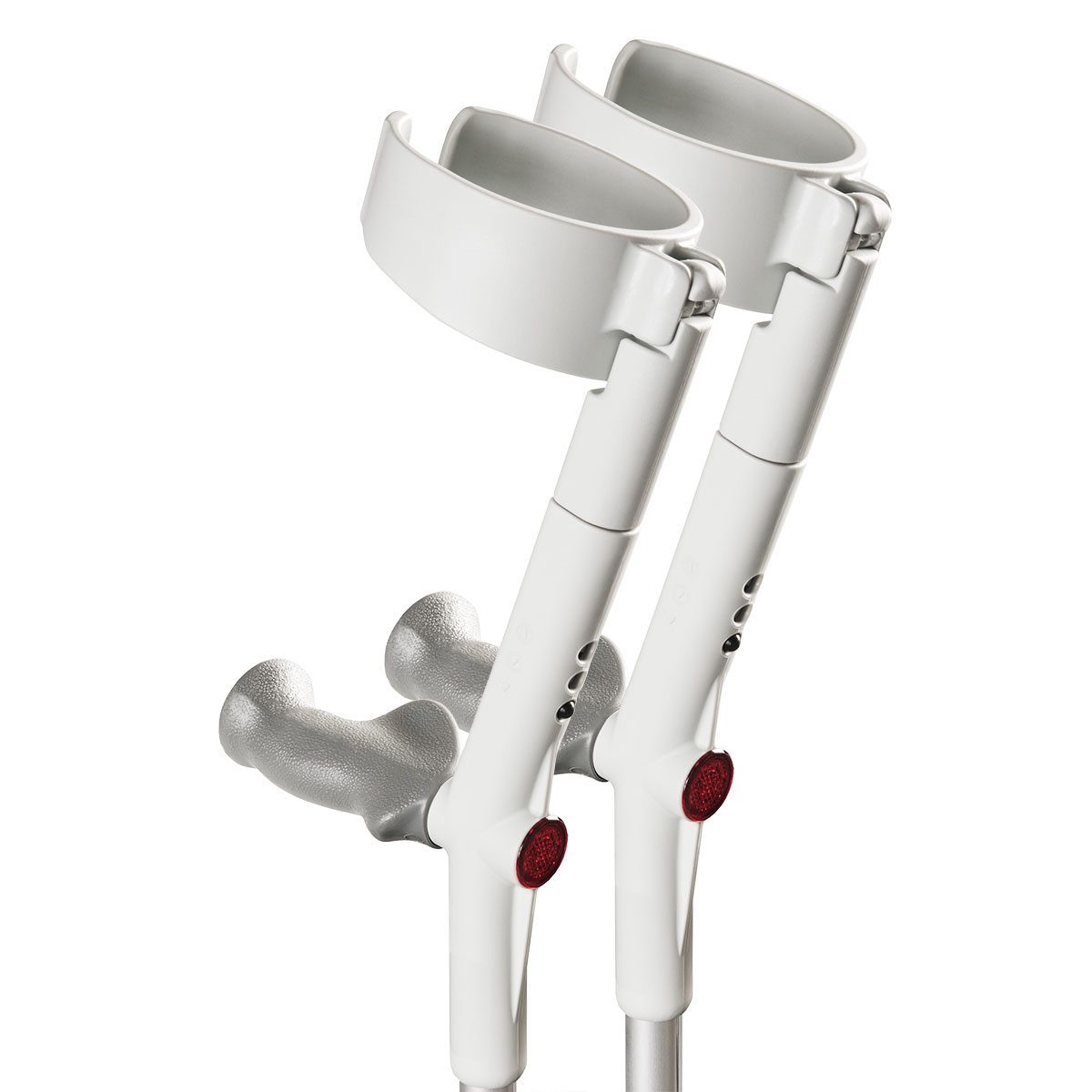
So easy to deal with, placed my order on line & my forearm crutches arrived 2 business days later! Everyone at hospital loved my crutches & the Physiotherapist even asked for the details of where … More I got them!
-
 Janet Williams
★★★★★
2 weeks ago
Janet Williams
★★★★★
2 weeks ago
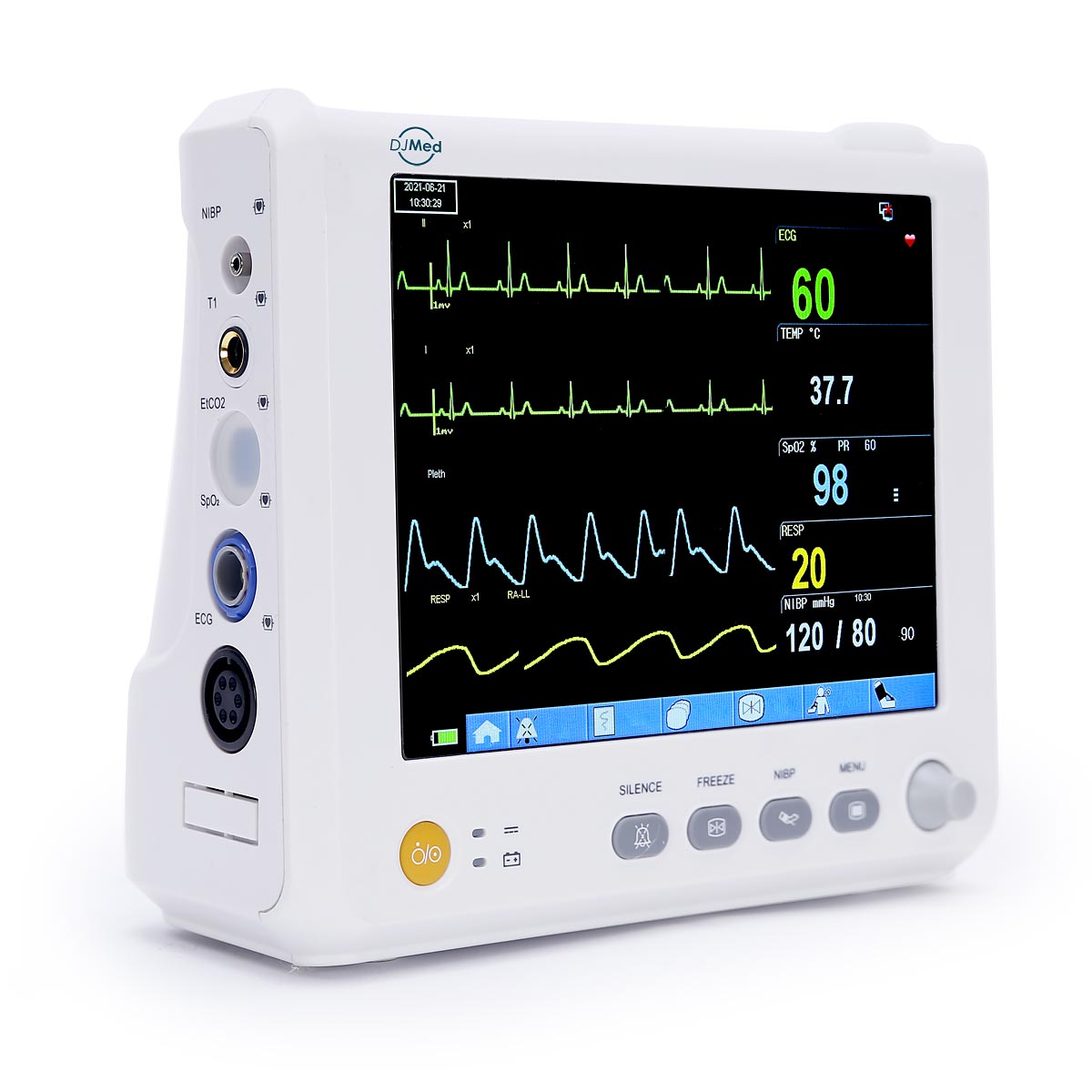
I received the items in a good time frame. They were just as described, easy to use and accurate. I can now how peace of mind checking the health of my family
-
 Damien Kelly
★★★★★
6 months ago
Damien Kelly
★★★★★
6 months ago
Fair price, very good quality. Easy to assemble and with a prompt delivery. I recommended to a friend earlier today.